Birth trauma can sometimes affect a newborn’s brain, especially after a difficult or delayed delivery. Early signs such as poor feeding, low activity, or unusual movements require immediate attention.
A quick evaluation by a pediatric neurosurgeon helps identify the issue, initiate timely care, and reduce long-term complications—giving your baby the best possible chance at healthy development and recovery.
When red flags appear, families often seek evaluation from Dr Rohit Mishra, an experienced pediatric neurosurgeon in Kolkata, for timely diagnosis and care planning.
The uncomfortable truth: some newborn symptoms are “normal”—some are not
Not every newborn symptom is harmless. While some changes settle on their own, others quietly signal a deeper problem.
Reassurances like “babies do that” can postpone action, especially when early newborn brain injury symptoms closely resemble normal newborn behaviour.
If something feels off, persists, or worsens, it’s worth getting checked early—because timing can change outcomes.
Why early action matters
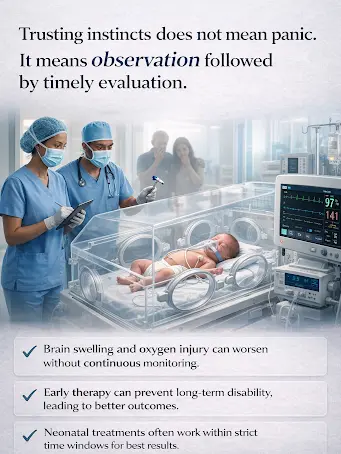
In birth trauma and newborn brain injury, time isn’t a buffer—it’s a turning point.
Early evaluation helps detect hidden injury, start targeted care, and reduce long-term impact. Acting quickly can protect brain development, improve recovery, and change a child’s future trajectory.
More reasons to not delay early care
- Brain swelling and oxygen injury worsen without monitoring
- Early treatment can prevent lifelong disability
- Many neonatal therapies work within narrow time windows.
What counts as birth trauma vs newborn brain injury?
Birth trauma involves physical injury during delivery. Brain injury involves oxygen deprivation, bleeding, or circulation problems affecting the brain. Both require medical evaluation, but differ in their causes and treatments. Families frequently confuse the two.
Birth trauma (physical injury during delivery)
Birth trauma refers to injuries caused by mechanical forces during labour.
Examples include:
- Bruising or scalp swelling
- Shoulder nerve injuries
- Skull fractures (rare)
Doctors may identify birth trauma in newborn cases during examination shortly after delivery. Most physical injuries heal with monitoring. However, swelling or bleeding must always be assessed carefully.
Brain injury (oxygen/blood flow issues or bleeding in/around the brain)
This includes:
- Oxygen/blood flow issues
- Internal bleeding in/around the brain
A strong example is hypoxic ischemic encephalopathy (HIE) newborn, a condition caused by reduced oxygen or blood supply during labour or delivery.
Unlike surface injuries, brain injuries may initially appear subtle.
Common causes of newborn brain injury linked to delivery

Lack of oxygen during birth (HIE) in simple terms
Oxygen fuels brain cells. Even short interruptions can trigger damage.
Doctors watch closely for:
- Delayed crying
- Weak muscle tone
- Poor breathing effort
HIE symptoms in newborns often include feeding difficulties or extreme sleepiness.
Another major warning factor is a low Apgar score, which is associated with increased risk of brain injury. A low early score does not confirm injury but signals the need for observation.
Early neurological consultation becomes essential when concerns arise. Families frequently seek advanced neonatal assessment from a pediatric neurosurgeon when oxygen-related complications are suspected.
Bleeding in/around the brain (intracranial haemorrhage)
Bleeding may occur due to fragile vessels or difficult delivery pressure.
Watch for:
- Irritability
- Seizures
- Weak crying
Parents searching online often encounter terms like intracranial haemorrhage newborn symptoms, which include poor feeding and abnormal breathing. Brain imaging helps confirm the diagnosis quickly.
Scalp bleeding that can become dangerous (subgaleal haemorrhage)
Scalp swelling sometimes appears harmless. But in subgaleal haemorrhage newborns, bleeding spreads beneath the scalp layers and may lead to significant blood loss.
Warning signs:
- Boggy swelling moving across the scalp
- Pale skin
- Increasing sleepiness
When instrument-assisted delivery increases risk (vacuum/forceps)
Vacuum or forceps deliveries can be safe when used appropriately. However, they increase monitoring needs afterwards.
Doctors assess:
- Head swelling
- Neurological tone
- Feeding ability
Observation during the first 48 hours matters most.
Risk factors doctors look for during labour and delivery
Prolonged/obstructed labour, fetal distress, emergency C-section
Common triggers include:
- Cord compression
- Placental problems
- Sudden fetal heart rate changes
Prematurity/low birth weight
Premature babies have fragile blood vessels. Even minor stress can cause bleeding or oxygen instability. Monitoring becomes essential during the first weeks.
Maternal factors (infection or severe BP issues)
- Severe hypertension (high blood pressure): Can affect placental blood flow
- Infections during pregnancy: May impact fetal health and oxygen delivery
- Placental inflammation: Disrupts nutrient and oxygen exchange
An early specialist review by Dr Rohit Mishra, a pediatric neurosurgeon in Kolkata, enables a more thorough neurological evaluation.
Signs you should never “wait and watch” at home
Seizures, breathing pauses, feeding failure, or spreading scalp swelling are emergencies in newborns. Immediate hospital evaluation protects brain function during the most vulnerable developmental stage.
Parents often recognise something is wrong before medical confirmation arrives.
| Category | Key Warning Signs | Implications |
| Abnormal Movements | – Newborn seizures after birth– Abnormal stiffness or floppiness- Extreme sleepiness | Signals oxygen instability; requires urgent hospital care after birth. |
| Breathing and Color Changes | – Breathing pauses (apnea)- Blue lips or repeated colour changes- Weak crying | Indicates severe neurological distress needing immediate monitoring. |
| Feeding Red Flags | – Cannot suck properly- Chokes repeatedly- Vomiting with lethargy | Poor feeding is an early neurological clue, often linked to brain oxygen issues. |
Scalp swelling that spreads quickly or looks boggy
Swelling that appears soft, boggy, or rapidly spreads across the scalp raises suspicion for subgaleal bleeding. Because it can progress quickly and lead to significant blood loss, urgent medical evaluation is critical.
“Is this normal newborn behaviour or a danger sign?”
Some newborn behaviours look alarming yet remain harmless. Others require emergency care. Comparing patterns helps families recognise when reassurance ends, and medical action must begin.
Normal variations vs urgent red flags
| Normal Variation | Urgent Red Flag |
| Brief startle reflex | Repetitive rhythmic jerking |
| Mild jitter when crying | Persistent limpness |
| Sleepy but wakes to feed | Difficult to arouse |
| Short irregular breathing | Long breathing pauses |
Babies recovering from oxygen stress may require monitoring inside specialised units providing NICU care for newborn brain injury.
What specialist care looks like (so parents aren’t terrified by machines)
Specialist newborn care focuses on monitoring brain activity, breathing, and circulation. Machines support recovery while doctors continuously evaluate neurological responses and prevent secondary injury.
Who gets involved
- Neonatologist
- NICU nurses
- Pediatric neurologist
- Neurosurgeon when required
Complex cases benefit from speaking to Dr Rohit Mishra, a pediatric neurosurgeon in Kolkata, for coordinated decision-making.
Tests commonly used
- Continuous brain activity monitoring (EEG)
- Ultrasound imaging
- MRI scans
Treatment options (what can be done, and when it matters most)
Therapeutic hypothermia (cooling therapy)
One of the biggest breakthroughs is therapeutic hypothermia cooling therapy for newborn treatment. Doctors gently lower body temperature. Why? Simply because cooling slows brain metabolism and reduces the spread of injury.
Important facts parents should know:
- Must begin within hours after birth.
- Requires specialised monitoring.
- Not every baby qualifies.
Early referral from a pediatric neurosurgeon ensures rapid decision-making when neurological complications arise.
Seizure control and breathing support
Stabilisation protects healing brain tissue.
What involves:
- Anti-seizure medication
- Oxygen therapy
- Ventilator support if required
Managing bleeding and shock
Some cases require surgical evaluation when the bleeding pressure increases.
Doctors monitor:
- Blood pressure
- Blood loss
- Brain swelling
What recovery can look like (realistic, not scary)
Recovery varies widely. Many babies improve completely with early treatment. Others require therapy and follow-up support. Honest expectations help families prepare without fear or false reassurance.
Mild vs moderate vs severe outcomes
- Mild injury may show full recovery.
- Moderate injury may require therapy.
- Severe injury needs long-term support.
Patients and families in the ‘City of Joy’ seeking long-term neurological guidance, many continue follow-up with Dr Rohit Mishra, a trusted pediatric neurosurgeon in Kolkata, to monitor healing progress and obtain developmental imaging when needed.
Why early therapy makes a difference
In newborn brain injury, early therapy can shape how the brain heals and adapts.
Starting care within the right window supports development, improves function, and reduces long-term challenges—making timely intervention one of the most powerful steps in recovery.
Early therapy includes:
- Physiotherapy
- Feeding therapy
- Occupational therapy
Developmental milestones to monitor
During the first year, watch for:
- Head control
- Rolling milestones
- Feeding coordination
- Social responsiveness
Early delays do not define the future. Intervention changes trajectories.
When to book a follow-up even if the baby looks “fine now”
After birth trauma, not all problems show up immediately. Some signs appear days or weeks later. Even if your baby seems well, a follow-up helps detect subtle changes early—when intervention is most effective, and outcomes are strongest.
Subtle signs appearing later
- Tone issues
- Poor feeding
- Delayed milestone
Follow-up schedule basics
- 1-month neurological review
- 3-month developmental check
- Imaging, if required
People Also Ask
Can a baby have a brain injury even after a normal delivery?
Yes. Oxygen fluctuations or bleeding may occur even after uncomplicated labour. Symptoms sometimes appear hours later, making post-delivery observation extremely important.
What is HIE, and how quickly must treatment start?
HIE occurs when the oxygen supply is reduced around the time of birth. Cooling therapy ideally begins within 6 hours to protect brain cells and significantly improve neurological outcomes.
Are newborn jitters the same as seizures?
No. Jitters stop when the limb is held gently. Seizures continue in a rhythmic pattern and may involve eye deviation or breathing changes, requiring urgent evaluation.
What does subgaleal haemorrhage look like?
It appears as soft, spreading scalp swelling that crosses head boundaries. Babies may quickly become pale or sleepy. Immediate hospital care is essential.
When should we go to the ER vs call the paediatrician?
Go to emergency services immediately for seizures, breathing pauses, blue episodes, or extreme sleepiness. Call a paediatrician for feeding concerns or mild behaviour changes.
Final Takeaway: Trust your instincts—and get the right team involved early

Babies cannot describe pain. They communicate through changes in feeding, movement patterns, and breathing behaviour.
If something doesn’t feel right, don’t wait. Subtle signs can matter. Early specialist care helps detect hidden issues, start timely treatment, and protect your baby’s development. Acting early isn’t overreacting—it’s giving your child the safest possible start.
Speak to Dr Rohit Mishra, a trusted pediatric neurosurgeon in Kolkata, without hesitation.